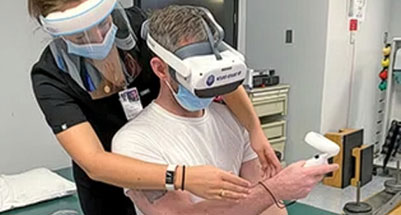
Understanding Veteran Traumatic Brain Injury
Traumatic brain injury (TBI) is a critical concern for veterans, making awareness and access to support and resources essential. This page is dedicated to providing valuable information and resources to veterans, their families and those interested in understanding the complexities of TBI. Here, you’ll find information about the signs and symptoms, diagnosis and treatment, prevention and risk reduction, and daily life impact of this condition.
About traumatic brain injury
Traumatic brain injury is a serious condition that affects an individual’s physical, cognitive and emotional health. It occurs due to a sudden jolt or blow to the head, leading to brain damage. Unfortunately, TBIs are prevalent among veterans due to the dangerous nature of military service.
Combat-related incidents, such as explosions or direct impacts from projectiles, are major causes of TBIs in veterans. Additionally, accidents during training exercises or active duty contribute to the risk. The Department of Veterans Affairs estimates that 15%–20% of veterans who served in Iraq and Afghanistan have experienced a TBI. The severity of these injuries can range from mild to severe, with long-term effects on health and well-being.
Signs and symptoms
Recognizing the signs and symptoms of traumatic brain injuries in veterans is crucial for early intervention and effective treatment. TBIs can manifest through various physical, cognitive and emotional symptoms.
Common signs and symptoms of TBI in veterans include:
- Physical effects: Headaches, dizziness, nausea, fatigue, sleep disturbances, and sensitivity to light or sound.
- Cognitive effects: Memory problems, difficulty concentrating, confusion, slowed thinking and trouble with decision-making.
- Emotional effects: Mood swings, irritability, depression, anxiety and changes in personality.
It is essential to understand that symptoms can vary in severity and may appear immediately or develop over time. Prompt medical attention is vital if you suspect a veteran may have a TBI, as early diagnosis and intervention can significantly improve outcomes.
Diagnosis and treatment
Accurate diagnosis and effective treatment of traumatic brain injury are critical for the well-being of veterans. Health care professionals use a variety of diagnostic methods, including neurological exams, imaging tests like CT and MRI scans, and cognitive assessments. These tools help determine the presence and severity of TBI.
Treatment options for veterans with TBI are extensive. Medications may be prescribed to manage symptoms such as headaches or seizures. Physical therapy can aid in improving mobility and coordination, while occupational therapy focuses on enhancing daily functioning and independence. Cognitive rehabilitation programs are also available to help veterans regain cognitive skills, memory and problem-solving abilities.
Support services are essential in the recovery process. That’s why DAV offers free claims assistance and helps veterans navigate the Department of Veterans Affairs system. Access to veterans benefits can not only provide health care and disability compensation but also adaptive equipment. These services aim to provide comprehensive support for veterans with TBI and their families.
Living with a TBI can cause great challenges, but organizations like DAV are ready to help.
Prevention and risk reduction
Preventing traumatic brain injuries in veterans is crucial for their safety and quality of life. Implementing preventive measures, education campaigns and safety protocols can significantly reduce the risk of TBIs.
One key preventive measure is prioritizing safety during physical activities. Veterans should be educated on the importance of using protective gear, such as helmets, during high-risk activities. Following safety guidelines and taking precautions to minimize the risk of falls, such as using handrails and maintaining a clutter-free environment, are also vital.
Education and awareness campaigns play a significant role in preventing TBIs. By providing accessible information about the causes, symptoms and consequences of TBIs, veterans and their families can recognize signs early and seek timely medical intervention.
Implementing safety protocols and providing appropriate equipment are also crucial. In health care settings, strict safety measures should be in place to prevent accidents. The use of safety equipment, such as bed alarms and fall mats, can reduce the risk of TBIs. Similarly, in homes and recreational facilities, ensuring the availability and proper use of safety equipment can prevent falls and subsequent TBIs.
Impact on daily life
Traumatic brain injury can have a profound impact on a veteran’s daily functioning and quality of life. The effects of TBI vary depending on the severity and location of the injury, but they can be long-lasting and significantly affect various aspects of life.
Veterans with TBI often face challenges in their daily routines and activities. Physical and cognitive issues may require adjustments in work, education and social interactions. Simple tasks that were once effortless may become difficult, leading to frustration and a sense of loss.
Cognitive issues, such as memory problems, difficulty concentrating and reduced problem-solving abilities, can hinder daily functioning. Physical symptoms like headaches, dizziness and fatigue further complicate daily activities.
To cope with the long-term effects of TBI, veterans can use various strategies. Rehabilitation programs, including physical, occupational and speech therapy, can help regain lost skills and improve overall functioning. Assistive technologies, such as memory aids or smartphone apps, can support managing daily tasks and schedules.
Establishing a supportive network of family, friends and fellow veterans is crucial. Joining support groups or engaging in counseling can help with navigating the challenges and emotions associated with TBI. Seeking professional help and asking for support when needed is essential.
At DAV, we understand the effect of TBI on veterans’ lives. Our organization is dedicated to providing resources, support and advocacy for veterans with TBI and other disabilities. Through our programs and services, we aim to enhance their quality of life and help them overcome daily challenges.
Support and resources
Community resources and support networks tailored to veterans and their families offer a sense of belonging and understanding. Local veterans organizations, such as DAV chapters, provide support groups, social events and networking opportunities to foster a supportive community.
At DAV, we are dedicated to helping veterans with traumatic brain injury access the support and resources they need. Our website provides comprehensive information about available programs, benefits and community resources. We encourage veterans and their families to explore these resources and reach out for assistance.
Recent research hints at the trove of information researchers are working to uncover.