New fees, structure for health care system

Changes are coming in the new year for those using TRICARE for their health care needs.
Beginning Jan. 1, 2018, the Military Health System will implement changes to modernize TRICARE in response to updates in law and policy. The following information outlines how the changes will impact TRICARE beneficiaries.
What are the key changes to note?
TRICARE Standard and TRICARE Extra will merge into one single plan, known as TRICARE Select. Certain enrollees will be able to obtain care from any TRICARE-authorized provider without a referral, and enrollees who obtain services from TRICARE network providers will pay lower cost-share amounts for in-network care.
All current TRICARE beneficiaries will be automatically enrolled in their respective health care plans on Jan. 1, 2018. Users of TRICARE Prime will be enrolled automatically in TRICARE Prime, and those currently enrolled in either Standard or Extra will be automatically enrolled in TRICARE Select. No action is required by beneficiaries, and enrollees are able to disenroll from any TRICARE plan at any time.
It is important to note that failure to enroll in TRICARE Prime or TRICARE Select (unless users are allowing existing coverage to automatically remain in force) will result in termination of coverage for civilian care. Those beneficiaries choosing not to enroll may only receive care at a military clinic or hospital on base, as available.
Beneficiaries can opt to enroll or change their plan during a yearly open enrollment period from November to December 2018, or following a qualifying life event.
Additionally, TRICARE will continue to provide a range of health care plans to meet beneficiaries’ needs, including premium-based plans like the Continued Health Care Benefits Program, TRICARE For Life, TRICARE Retired Reserve, TRICARE Reserve Select and TRICARE Young Adult.
Will current beneficiaries be grandfathered?
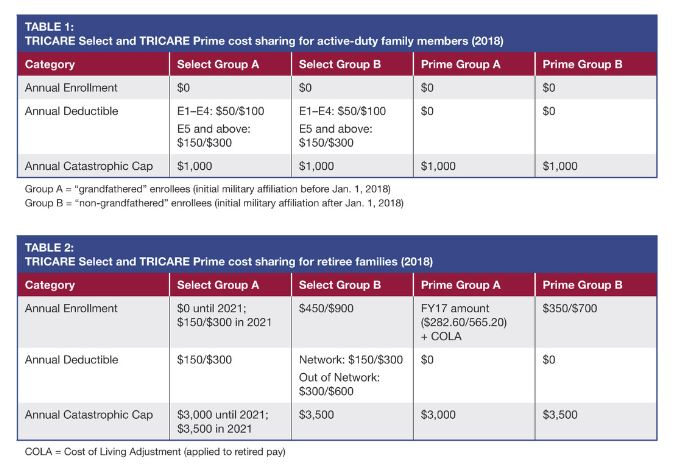
All enrollees whose sponsors’ military affiliation began before Jan. 1, 2018 (all current beneficiaries) will fall under Category A and are considered grandfathered for new enrollment fees and out-of-pocket costs, in accordance with the current law. Those whose sponsor’s military affiliation begins after Jan. 1, 2018, are in Group B and are considered not grandfathered.
Tables 1 and 2 list anticipated changes to enrollment fees and other cost-sharing expenses for current active-duty families (Table 1) and retiree families (Table 2).
What changes will occur during transition from fiscal year to calendar year administration?
TRICARE will also change from a fiscal year (October to September) period to a calendar year (January to December) period, aligning with open enrollment. To protect beneficiaries from incurring additional costs, enrollment fees will be prorated for the three-month period between Oct. 1 and Dec. 31, 2017.
Payments that would normally count toward catastrophic caps and deductibles until Oct. 1 will continue to count until Jan. 1, 2018. Enrollees who reach their fiscal year 2017 catastrophic caps will not incur additional out-of-pocket costs for authorized TRICARE-covered services during the last three months of 2017.
What can you do to prepare?
- Check and update your current information in DEERS, to include your contact information and any significant life events such as military activation, separation or retirement, marriage, divorce, or the birth or adoption of a child.
- Sign up for benefit updates at tricare.mil/changes.
- Update your payment information if you are using electronic payments.
For the latest information on these and all TRICARE changes, visit tricare.mil/changes.