Through VA-funded research, veterans become first Americans to undergo new prosthetic limb operation

After a decade of preliminary research, two veterans are participating in an important and cutting-edge clinical trial that could change the lives of veteran amputees and reinvent the way we think about prosthetics.
In December 2015, Army veterans and amputees Bryant Jacobs and Ed Salau were the very first Americans to receive Percutaneous Osseointegrated Prosthesis, or POP, implants at the Salt Lake City VA Health Care System.
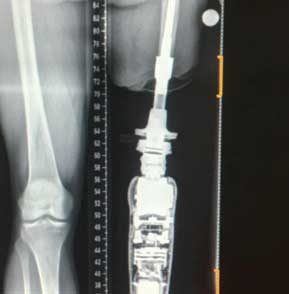
Typically, amputees cap their truncated limbs with a latex sock and put it straight into a socket. The POP implant removes the need for a socket by surgically inserting a titanium rod into the patient’s femur before attaching a docking station for the new limb. This offers more comfort and range of movement.
For many amputees, the socket attachment is difficult to wear for more than a few hours a day. It also oftentimes causes sweating, pain and frequent trips to the doctor for refitting if the wearer’s weight fluctuates.
“Every problem with my prosthetic limb is related to my prosthetic,” said Salau, who lost his left leg in Iraq in November 2004 when a rocket-propelled grenade hit the vehicle in which he was riding.
“I’ve had open sores this whole time,” agreed Jacobs, whose right leg was amputated two years ago after a decade of complications from the injury he received from a roadside bomb in Iraq. “Its just stuff like that that impedes life, like putting on jeans. The IED blew most of my inner thigh out, so I have a lot of bone Growth in that area, so a socket fit is really hard. Every 20 minutes I’d be dripping in sweat.”
“Over half of the people that have amputations from blast injuries—that means all of our veterans—have bone in their muscle and their soft tissue,” said Dr. Laurence Meyer, director of research at the Salt Lake City VA. “And when we get that socket pressing on that, it limits the amount of time they can wear the socket, or it means they can’t move at all.”
The new POP implant surgery is a part of a VA-funded clinical trial approved by the U.S. Food and Drug Administration to determine the safety and function of the new implant. The Salt Lake City doctors had special permission to perform the procedure, which has been done in other countries but never legally in the U.S.
“The big advantage with osseointegrated prosthesis is getting rid of the socket, as 50 percent of them have problems,” said Dr. Rickard Branemark, associate professor at the University of California, San Francisco, School of Medicine.
Branemark’s father, Swedish bioengineer Per-Ingvar Branemark, discovered osseointegration in the 1950s. While implanting titanium cylinders into rabbit femurs, he found he couldn’t extract the titanium without destroying the surrounding bone.
“What seems to be happening is titanium fuses with live human bone,” said Branemark. “The difference is in the way it connects to bone tissue—rare that it fades over time, as it’s a robust connection to the bone. With osseointegrated prosthesis they can be much more mobile—no socket means they can sit down and rotate their leg. They cannot do that with a socket because their leg would fall off.”
The experimental surgery is a two-phase operation. Salau and Jacobs underwent surgery Dec. 7, 2015, to implant titanium rods into the base of their femurs. Then on Feb. 8, the surgeons attached a docking mechanism for a prosthetic leg to the titanium rod.
In April, Salau and Jacobs attached their new legs and stood up.
“I can feel the ground,” said Salau. “I haven’t had that sensation in 11 years. I wanted everything better, faster, smoother—that’s what I think I have now. It’s a Big game-changer. I found there were no more blisters. There was no more skin irritation. I just walked around.”
“I have a leg again,” said Jacobs. “As soon as the stitches came out, it was easy. There was nothing going on. There was no pain. It was almost like you couldn’t tell you have it. Everything is 100-percent different, but better.”
There are even more potential upsides to a POP implant than the current latex sock and socket prosthesis, including “osseoperception,” the adjustment of the mind to an osseointegrated prosthesis.
“The implication is that bone-integrated prosthetic fixtures communicate with the mind, via numerous neural pathways, to promote near-normal function and improved psychological acceptance,” said Dr. Robert Myers, professor emeritus of anesthesiology and neuropathology at the University of California, San Diego. “A patient may be able to sense, through their artificial leg, what type of subfloor was beneath a carpet.”
Salau acknowledges a greater sense of feel and believes the surgery could make a huge difference in the way newly amputated veterans cope with their new lives.
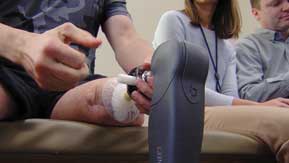
“Sitting here, I can feel the slightest indentations in the tile beneath my feet,” he said. “In the future, because of this, we will wake up from an accident or a trauma in combat and we will have a rod inserted and we will be told in a few weeks, we will connect your limb and you can start walking again.”
Over time, the muscles in Jacobs’ and Salau’s legs will grow stronger as the titanium rod fuses with their bone, ultimately making it possible for them to move with relative ease.
“We’re excited to see the progress these veterans are making,” said Meyer. “These first steps are amazing for the patients and our team. This is a long-term study that will (eventually) cover 10 veterans over multiple years, and if successful, we hope it will be expanded to a larger number of patients.”
Although this is an exciting step forward, there are still many more phases of the research that will need to be conducted before FDA approval can be granted.
“This is a very exciting start to a very exciting process, and I am proud of our friends at the VA for funding such a trial,” said DAV National Commander Moses A. McIntosh Jr. “In the near future, we may be able to reduce some of the physical and mental stress, while speeding up the recovery for veterans forced to endure amputations. … However, for now we just want to continue to monitor the situation and hope for more progress and more good news coming back to the medical staff.”






