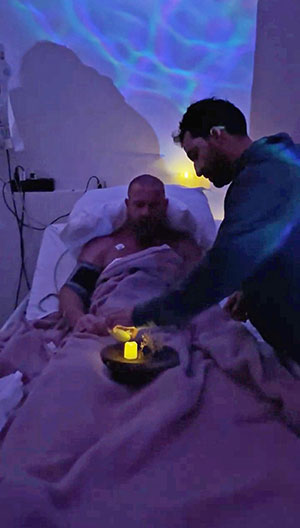
On a quiet morning in Cancún, Mexico, with monitors tracing the rhythm of his heart, Noah Galloway leaned back and prepared to surrender what had been crucial to his survival—control.
Galloway had come a long way since he graced the cover of Men’s Health magazine and was a finalist on ABC’s “Dancing With the Stars” in 2014. He enlisted in the Army after 9/11 and deployed twice with the 101st Airborne Division. In 2005, during his second tour in Iraq, an explosion cost him his left arm and leg. He returned home determined to push forward—physically, publicly, relentlessly.
He built a life on strength, showcasing resilience in public speaking. However, the foundation holding everything was built on silence.
“I bottled it all up,” he said. “Not just the injury. Everything.”
For years, he lived in extremes, either driven and outward-facing or withdrawn and shut down. Emotions, when they surfaced, often came out as anger. Sadness stayed buried. His nervous system never fully powered down.
“I was always in fight or flight,” he said.
Then, four years ago, his wife introduced him to psilocybin, a psychedelic used in clinical settings to treat depression, anxiety and addiction. The experience surprised him. Emotions he’d long suppressed began to surface. He cried. He reflected. He felt.
“That was the first crack in the armor,” said Galloway.
Over time, he tried several other therapies. Eye movement desensitization and reprocessing (EMDR). Neurofeedback. Ayahuasca in Peru through the Heroic Hearts Project. Later, 5-MeO-DMT, a powerful, short-acting medicine.
Each step, he said, built on the last.
But ibogaine felt different.
Derived from a West African shrub, ibogaine remains illegal in the United States and carries known cardiac risks. Treatment is often sought abroad under medical supervision. Galloway traveled to a clinic in Cancún, where patients undergo medical screening and are monitored continuously during the process.
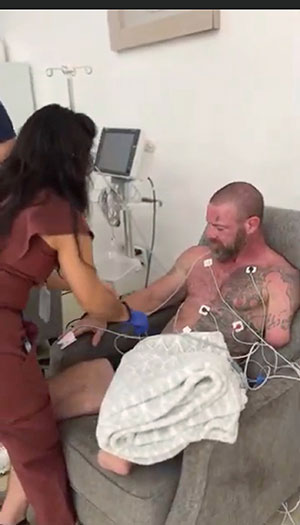
Unlike ayahuasca, which Galloway experienced ceremonially in Peru, ibogaine was administered with doctors and nurses present. He was connected to an electrocardiograph. An IV line was placed as a precaution.
“Ibogaine can affect your heart,” he said. “They monitor everything.”
The medicine also affects people in unique ways. For Galloway, the experience itself was less visual than he expected. No fireworks. No dramatic emotional purge.
“It removes the noise,” he said. “It resets your nervous system.”
Galloway is part of a mounting number of veterans seeking relief outside traditional channels as research into psychedelic-assisted therapies gains national attention.
Psilocybin, MDMA and ibogaine are some of the psychedelic compounds currently in clinical trials. Earlier studies—and mounting anecdotal reports—suggest they may help address treatment-resistant post-traumatic stress disorder, depression and moral injury. As lawmakers debate access and researchers push for clinical clarity, veterans are once again at the forefront of a conversation that could reshape mental health care.
For Galloway, the most meaningful changes weren’t what he saw in the moment but what followed.
Researchers studying psychedelic-assisted therapy say that pattern isn’t unusual.
“What we’re finding,” said Brandon Weiss, a researcher in psychedelic science at Johns Hopkins University, “is that certain features of the acute experience—particularly emotional breakthrough and shifts in self-understanding—are associated with longer-term symptom improvement.”
Weiss points to three recurring elements in studies of psilocybin and related compounds: emotional processing of traumatic material; the ability to observe one’s own thought patterns; and experiences often described as unity, meaning or profound perspective shifts.
“These experiences can allow people to examine long-held beliefs about themselves,” Weiss said, “especially beliefs rooted in shame or early life experiences.”
He cautions that the drug alone isn’t the intervention.
“Preparation and post-session support are critical,” he said. “The psychedelic can open things up. The support helps people integrate what they’ve seen.”
During his experience, Galloway said he saw humanity as part of a single tree, its branches reaching outward and its leaves representing people pulling from the same source. Some branches fought one another, unaware they were fed by the same trunk.
The image lingered with him, a reminder of how deeply connected and interdependent humans are.
He also experienced moments of distance, observing Earth from above and feeling disconnected from ego and performance. At one point, he describes floating alone in space—not afraid, not lonely but simply present.
“For someone with anxiety and PTSD, being alone with your thoughts is usually terrifying,” he said. “But I was OK.”
Friends noticed he seemed calmer. Less reactive. More grounded.
Before, small stressors could trigger outsized reactions followed by regret. Now, he finds space between stimulus and response.
While traveling recently, he called his teenage daughter about a situation that could have escalated.
“She was immediately defensive,” he said. “And I told her, ‘You’re not in trouble. We’ll talk about it later.’”
That pause—that regulation—felt new.
“When you’re calm, you get more accomplished,” he said.

Like many veterans, Galloway once believed his struggles stemmed primarily from combat.
But psychedelic work challenged that assumption.
Stress or moral injuries suffered in service can aggravate and elevate preexisting conditions.
“We have so much from childhood that shapes how we respond to trauma,” Galloway said.
Weiss said research increasingly supports that observation.
“Psychedelics can increase metacognitive awareness,” he said. “People begin to see how earlier experiences shaped their responses. They often move from self-criticism to self-understanding.”
In some cases, that shift reduces the secondary suffering layered on top of trauma—shame about having symptoms or anger at oneself for reacting a certain way.
“It doesn’t erase what happened,” Weiss said, “but it can change the relationship someone has to it.”
As interest in psychedelic-assisted therapy grows, some experts urge careful guardrails alongside optimism.
“These remain investigational interventions,” said Dr. Joseph Fins, chief of the Division of Medical Ethics at Weill Cornell Medicine. “They are not yet established treatments. That distinction matters.”
Fins, whose work focuses on neuroethics and emerging brain-based interventions, said psychedelics should be delivered within structured clinical frameworks with rigorous screening, medical oversight and long-term follow-up.
“You can’t simply open someone up and send them home,” he said. “The biological effects may be powerful, but without psychological support and continuity of care, you risk doing only half the work or potentially exposing someone to harm.”
For veterans in particular, he emphasizes that care must account for both individual trauma and group identity.
“Service members are shaped by unit cohesion and solidarity,” Fins said. “Treatment shouldn’t isolate them from that reality. Individual therapy is important but so is group connection—realizing your experience, while deeply personal, is not uniquely yours.”
He also raises a practical concern: What happens if these interventions prove successful?
“We often focus on whether something works,” Fins said. “But we also have to ask: If it works for you, then what? Who supports you long term? Once we begin, we have an obligation to finish.”
For veterans navigating hope alongside uncertainty, that balance—innovation paired with infrastructure—may be just as important as the medicine itself.
Ibogaine, like most psychedelic compounds, is still being studied. The Food and Drug Administration hasn’t approved it for any conditions. Access is limited. Risks exist, and patients must be carefully screened.
“We still don’t know long-term durability across populations,” Weiss said. “And we don’t have large-scale data comparing different integration models.”
He emphasizes that screening, monitoring and follow-up are essential, particularly in populations vulnerable to depression or suicidal ideation.
For Galloway, the experience was about enhancing rather than bypassing therapy.
“I used to think therapy didn’t work,” he said. “Now I realize it works when you’re willing to work.”
He continues to attend sessions. He treats ibogaine not as a cure but as an opportunity.
“My nervous system feels reset,” he said. “Now it’s on me to build new habits.”

Galloway believes veterans are uniquely positioned to shape how the country views emerging mental health treatments.
“I’ve said before, veterans are going to lead the way in mental health,” he said. “Because people can see the change.”
He has seen skepticism soften when lawmakers and community members hear firsthand accounts. He points to public figures who shifted their stance after meeting veterans reporting improvement.
But he’s careful not to oversell.
“Any therapy only does so much,” he said. “The work is in us.”
For a man who once measured strength by how much he could suppress, that may be the most profound change of all.
He no longer feels compelled to perform resilience. He wants something simpler now.
“I just want to live my best life,” he said.
And for the first time in decades, he said that life feels quiet enough to build.






