VA continues to introduce new pain management therapies to curb the opioid epidemic among veterans
According to a 2017 Department of Veterans Affairs inspector general (IG) report, in fiscal year 2016 the Veterans Health Administration (VHA) treated 190,381 patients with a diagnosis of a drug use disorder.
Thirty-five percent of those patients were abusing opioids.
But the opioid crisis seen in the VA—and throughout the country—did not happen overnight. According to the VHA Pain Management office, since the publication of the VA/DOD Clinical Practice Guideline for Management of Opioid Therapy for Chronic Pain in 2010, opioid misuse and opioid disorder have steadily grown across the nation.
Combatting a new enemy: the opioid epidemic
According a 2014 VA IG report, in fiscal year 2012 the VA provided nearly 2 million take-home opioid prescriptions to more than 450,000 patients. About one-third were classified as chronic users, based on the investigation findings. Almost 94 percent of those patients were diagnosed with either pain or mental health issues, and almost 60 percent were being treated for both.
The IG found that patients with six or more prescriptions were the majority of chronic opioid users and patients requesting early refills were not uncommon. Refills of opioids at least a week early occurred in 23 percent of the population studied in the report, and 14 percent of the prescriptions were refilled at least 11 days earlier than intended by the provider. The IG report determined this was an indicator of “high-risk opioid behavior.”
“Since the VA started aggressively tackling the opioid problem in 2014, we’ve been concerned with the rapid reduction in the VA’s prescribing of painkillers without clinicians first properly educating veterans about the dangers of long-term opioid use and talking about alternative treatment options to address chronic pain,” said DAVNational Legislative Director Joy Ilem.
The 2014 investigation further determined that 71 percent of patients who were prescribed take-home benzodiazepines were also given concurrent prescriptions of opioids—a potentially deadly combination.
“The concurrent use of benzodiazepines and opioids can be dangerous because opioids and benzodiazepines can depress the central nervous system and thereby affect heart rhythm, slow respiration and even lead to death,” the report states.
Monitoring the patients who were prescribed opioid therapy was also an issue, the IG found. Only 37 percent of opioid patients were administered a urinalysis for drug abuse coupled with a six-month follow-up with their physician.
According to Psychology Today’s Eric Newhouse, citing a 2016 VA IG report, between 2010 and 2015, the number of veterans addicted to opioids rose by more than half.
“Millions of veterans enrolled in VA health care have been aided by the VA’s efforts to better manage pain through alternative therapies; however, a number of veterans with chronic pain who have been prescribed pain medication over long periods reported they were abruptly denied further access to prescription medications for pain with little explanation,” Ilem said.
Ilem said that without appropriate education, psychological counseling and transition to suitable alternatives to control chronic pain, as recommended by VA policy, veterans can needlessly suffer physical and mental anguish.
“While we support the VA’s efforts to increase alternative nonpharmacological approaches to pain management, these therapies are not consistently available at all VA facilities. Additionally, we urge continued research efforts to ensure the efficacy of these interventions in managing severe, often debilitating chronic pain—especially for war-related trauma and injuries,” said Ilem.
Changing how we treat pain
In February 2017, the VA published version 3.0 of the VA/DOD Clinical Practice Guideline for Opioid Therapy for Chronic Pain, which was prepared by the Opioid Therapy for Chronic Pain Work Group and based on evidence gathered through the end of last year.
According to the guide, today the VA recommends strongly against using long-term opioid therapy for chronic pain, advocating instead for alternatives to opioid therapy that include nonpharmacological treatments and—if pharmacological treatments are used—prescribing non-opioid medications rather than opioids. If a medical provider does determine opioids should be prescribed for chronic pain, the guidelines strongly advocate for short-term treatment.
“The accumulation of evidence of harms and the absence of evidence of long-term benefits has warranted a newly cautious approach to [long-term opioid therapy] that prioritizes safety,” according to the VA’s guidelines.
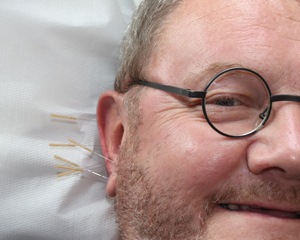
Battlefield acupuncture—one alternative to opioids
Dr. Richard Niemtzow said he designed a treatment he calls “battlefield acupuncture” (BFA) in August 2001 while at the Naval Medical Center in San Diego.
Niemtzow said the Air Force has been teaching physicians BFA prior to deployment to Iraq and Afghanistan since 2009.
“In battle, special forces have used BFA in circumstances not requiring morphine,” Niemtzow said. “BFA does not reduce the respiratory rate as does morphine, [which] requires an observer to prevent respiratory deficiency. Also, BFA reduces the acute pain from tourniquets and substitutes for morphine.”
He said this nonpharmacologic form of therapy is easy to learn and can produce rapid pain relief. He also said it has been prescribed to help patients break the opioid habit.
“I designed it to entail the placement of semi-permanent needles into five specific ear points on the exterior surface of both ears,” Niemtzow said. “In many cases it reduces pain when standard therapies have failed.”
Niemtzow said the favorable response rate for patients using BFA to combat pain is 70 percent.
But this technique is not without its naysayers. In a 2011 article in Forbes, Dr. Steven Salzburg called BFA “pseudoscience” and “the worst quackery of the year.”
“Multiple scientific studies have shown clearly that acupuncture doesn’t work,” reported Salzburg, a professor of biomedical engineering, computer science and biostatics at Johns Hopkins University. “The benefit is the same no matter where you place the needles, or even if you use toothpicks that don’t pierce the skin. Acupuncture points and meridians—the pathways that acupuncturists claim to manipulate with their needles—don’t even exist.”
While Niemtzow acknowledges BFA is not a “cure-all” for pain relief, it has been used successfully in many scenarios.
“Patients achieve either a short- or long-term benefit based on their pathology,” he said. “BFA has become the most popular employed ear pain modality in the armed forces. In order to minimize the use of opioids as an initial treatment, BFA is offered as a safer alternative medicine.”
Battlefield acupuncture and veterans
“Over the course of a 30-year career in neurology, I had lost enthusiasm for seeing patients in pain, particularly those with headache, as I had little to offer than yet another manipulation of medication,” said Dr. Michael Freedman, a neurologist with the Durham Veterans Affairs Medical Center Greenville Health Care Center.
While there may be debate over the efficacy of alternative therapies, clinicians within the VA are working to find the best, safest combination of solutions to help their patients manage chronic pain. And Freedman, among other doctors, has reported notable successes for patients.
“The VA has steadily introduced complementary and alternative medicine options for patients, and acupuncture is just one of the methods that—in a closely monitored clinical care setting—has been showing some promise,” Ilem said.
In 2016, Freedman performed nearly 600 acupuncture treatments, with 345 using BFA or BFA in conjunction with other acupuncture techniques. Freedman said less than 10 patients reported no relief in pain after undergoing acupuncture treatment.
“It’s a way of relieving pain without taking opiates,” said Freedman. “Battlefield acupuncture reduces pain, so it’s intuitive that you’ll need less pain medication. There’s a huge area of opportunity here in training VA [doctors] in BFA and acupuncture techniques.”
Freedman said he hopes the VA will increase funding and credential providers to deliver acupuncture treatments as these methods are simple, safe, inexpensive and—according to his findings—effective. And while he says acupuncture should be only one of many tools to combat the opiate epidemic among veterans, he strongly advocates acupuncture as an adjunctive treatment to combat the opioid problem.
“There’s a lot of talk about dealing with the opioid crisis and not a lot of talk on how to do that,” Freedman said. “Acupuncture is just sitting there.”
“VA needs to explore nonpharmacological alternatives like acupuncture for managing pain and continue research efforts to ensure they are effective. We need to give injured and ill veterans the best possible chance at a higher quality of life, free of pain,” said Ilem.