For the harshest critics of the Department of Veterans Affairs’ Veterans Health Administration (VHA), the storyline often shared in the media is convenient to their cause. Reported long wait times and an annual budget of $142.4 billion offer a target for outrageous headlines that call for VHA’s demise.
But these views contradict academic studies, patient experience surveys and VHA employee consensus that the health care system developed to care for our nation’s veterans is, in fact, high quality and irreplaceable.
Through VHA, the VA operates the largest integrated health care system in the country, with 170 medical centers and 1,193 outpatient clinics serving 9.1 million veterans. The demand for services in recent decades has grown primarily due to increases in aging veterans and in the number of veterans with more disabling conditions who would have died, as in previous military conflicts, if not for advances in battlefield medicine.
“While the majority of Americans agree that the nation should honor its sacred obligation to take care of those who have ‘borne the battle,’ few understand the potential ramifications to disabled veterans and their families, health care professionals and the nation at large if VHA were to no longer exist,” said Washington Headquarters Executive Director Randy Reese.
Veterans Access to Care
If the VA’s health care system were to completely shut down, disabled veterans would be forced to seek all of their care in the private sector.
But could the private sector handle this massive influx?
Like VHA, the private system is already understaffed and overwhelmed. Kaiser Family Foundation data from 2024 shows that more than 7,400 locations in the United States and its territories have health care provider shortages, affecting more than 74.3 million people. Foundation data also shows that 122.2 million people are now affected by a provider shortage in mental health care, with only 26.8% of that need being met.
Moving more than 9 million veterans from VHA to private health care doesn’t solve the staffing problem; it just shifts the responsibility to an already strained private system. The problem is more pronounced in rural areas, where almost 25% of veterans—about 5 million of them—live.
Yet advocacy for full privatization persists.
That was the initial position of former VA Secretary Dr. David Shulkin when he became the VA’s under secretary for health in 2015 before his 2017 confirmation as secretary. He first came to the department under the Obama administration with years of experience running private hospitals and self-admittedly had limited knowledge of the VA system.
But after learning how much veterans valued the care they received and coming to understand the VA health care system, Shulkin had a change of heart.
“I became one of the strongest advocates for maintaining and strengthening the VA system for one simple reason: It was the right thing to do to honor our commitment to our veterans,” Shulkin said.
Shulkin left the government in 2018 but remains a vocal advocate for VA health care while also endorsing the MISSION Act, legislation that established the VA’s community care program and veterans’ right to choose where they receive their care. There may be circumstances where private care makes the most sense, but with a private care-only solution, he said, veterans would be bound to the rules and services set by insurance companies.
“[VA health care] is a much more comprehensive, holistic system of care that, frankly, serves veterans extremely well,” Shulkin said. “We don’t have to worry about whether an insurance company is going to pay for it. We worry about whether it’s the right thing to do.”
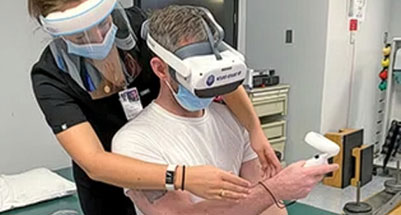
Because VHA isn’t bound by the constraints of insurance companies and profitability, its doctors can provide high-quality, specialized care even if it’s not economically viable to do so. Shulkin said that’s why integrated behavioral and mental health care, suicide prevention programs, toxic exposure environmental analysis programs, adaptive sports clinics, blind rehabilitation and other specialized offerings exist.
In situations where VHA may be the only source of specialized care for veterans—especially in rural communities where other medical care is often limited or far away—they still have access. Removing VHA would eliminate that choice, leaving veterans with fewer options for care.
“[In the private sector] there just aren’t subspecialists and there aren’t enough people who work in those parts of the country. And attracting qualified health care professionals to rural areas is challenging,” Shulkin said. “If we didn’t have a VA, that would be clearly an area where veterans would suffer.”
A hot-button issue that’s been highly publicized for many years is patient wait times at VHA facilities. If veterans hospitals were shuttered nationwide, veterans would likely see wait times increase when seeking care solely from private providers. In fact, studies comparing current wait times between VHA and private facilities show they are about the same, with VHA’s wait times trending down.
Quality of Care
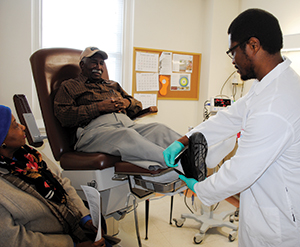
With more than 9 million enrolled veterans, VHA serves people whose lived military experiences are foreign to many civilian health care professionals. Essentially, disabled veterans are served by a system designed for them that has advocates and providers who know military culture, the unique challenges veterans face and the language they use.
Numerous academic studies have shown that care at VHA facilities is just as good or better in many cases than the private sector. If veterans were forced to move to private care, they would move away from a system that relies on evidence-based clinical care that leads to lower readmission rates and fewer post-surgical complications than civilian providers. They would also no longer see clinicians who spend more time with their patients and broadly utilize time-saving, convenient options like telemedicine when practical.
Electronic record sharing, something VHA innovated, enables every doctor and specialist a veteran may see to have access to the same medical information. When a veteran is seen in the community it is essential those records are integrated into VHA’s electronic health record for continuity of care. Unfortunately, private health care systems don’t always share electronic medical records, and when they do, integration of those records isn’t always seamless.
VHA offers a holistic approach for veterans in which medical providers know how certain conditions are linked to military service. For instance, if a veteran develops Type 2 diabetes and has Agent Orange exposure, the VA presumes the two are connected. That understanding is a strength of VHA, allowing veterans to receive treatment without having to prove the connection.
As a study in the journal Health Services Research notes, provider cultural competence in veteran-related health care issues is a complication to providing care. VHA providers specialize in understanding the specific needs of their patient population.
Losing VA health care would put veterans exclusively in the care of those who may not understand their military experience or unique medical needs and conditions.
“Our country has pledged to care for our veterans, and without VHA health care, the special attention given to them would disintegrate into one more government-funded reimbursement program where the background of presumptive conditions veterans face would be little known or considered,” said DAV National Legislative Director Joy Ilem.
Additionally, VHA providers ask all veterans about their housing, employment, food security and transportation situation during each appointment. When a veteran expresses having one of these needs, a referral is made to a VA or community program, which isn’t the case in the private sector.
Health Care Professionals and Medical Innovation
Training health care professionals—including physicians—is one of the VA’s four statutory missions. Since 1946, VHA has worked with academic institutions to provide high-quality, state-of-the-art health care to America’s veterans; train new health professionals; and advance health care practices and medical innovation.
According to the Association of American Medical Colleges, VHA is the largest provider of medical training in the U.S. and has become an irreplaceable component of the country’s medical education system. VHA supports over 120,000 trainees and students annually in affiliation with over 1,800 educational institutions for more than 40 different health professions, with nearly 70% of all U.S. physicians completing at least part of their training in VA facilities.
“It was an important part of my medical training both as a medical student and a resident,” Shulkin said. “It’s just one of the ways the VA contributes to improving health care, not only for veterans but for all Americans. This educational system is really an integral part of the way that health professional education happens in this country. If you speak to most people who have trained in the VA, they can tell you how impactful that training is.”
Besides playing an essential role in the way doctors are trained in the U.S., VHA’s impact has extended far beyond the veteran population it serves through a combination of education, research and patient care. Through this successful model of integrated care and collaboration, VHA has yielded groundbreaking treatments and state-of-the-art technology that has improved countless lives.
VHA researchers have helped pioneer innovations—the shingles vaccine, the implantable cardiac pacemaker, the first liver transplant—that benefit not only the American people but also countless others across the globe. In fact, the department holds over 600 medical patents.
“VHA has made itself indispensable within American medicine,” said Dr. Harold Kudler, associate consulting professor in the Department of Psychiatry and Behavioral Sciences at Duke University. “Our nation’s health system could not withstand its loss. Research, training and medical innovation dedicated to the special needs of our nation’s veterans would lose priority without it, and the public would be deprived of breakthrough discoveries which VHA is uniquely capable of achieving.”
More than 60% of VA researchers also provide direct patient care within the VA system, giving them firsthand insight into veterans’ health needs and enabling them to put their findings into practice more quickly. The uniqueness of the VA’s integrated health care system and research has produced three Nobel Prize winners for medicine or physiology in its ranks, along with recipients of seven Lasker-DeBakey Clinical Medical Research Awards and numerous other national and international honors related to medical research.
Additionally, VHA has embarked on one of the largest medical research studies ever, the Million Veteran Program (MVP), which looks at how genetics, lifestyle, military experience and toxic exposures affect health and wellness among veterans.
“MVP has the power to link genetic issues to diagnosis and responses to treatments and begins to create more predictive power to improve health outcomes,” Kudler said. “VHA can create a national model of whole health that can guide other health care systems to gauge overall well-being and improve health care and health outcomes for all.”
Take Action
 Health care for veterans isn’t a partisan issue—it’s part of a solemn promise the United States made to men and women who’ve served in its military.
Health care for veterans isn’t a partisan issue—it’s part of a solemn promise the United States made to men and women who’ve served in its military.
But in a political climate of divisive positions, the VA is an easy target when critics ignore the people the VA serves and focus only on the dollars and cents. At first glance, it’s a sizable budget and a tempting pool for Congress to skim from when they consider other initiatives, proposals and bills vying for resources.
“However, what must be top of mind for lawmakers, veterans and all citizens is how important and essential VA health care is for everyone in the United States,” said Reese. “VHA is not bound to the constraints of profitability, the bottom line or the whims of health insurance companies, which allows it to operate in the best interest of veterans and the general public. Training the next generation of the nation’s health care providers, developing innovative treatments and modeling the benefits of equitable access to quality integrated health care all come because VHA exists as it does.”
“A strong and viable veterans health care system is part of keeping our promise to those who served. Continued improvements to that system are essential and come because of a unified voice keeping lawmakers on Capitol Hill accountable to do what is right and best for veterans,” said Ilem.
DAV offers legislative advocacy support for everyone through DAV CAN (Commander’s Action Network), said Ilem. Through DAV CAN, anyone—not just DAV members—can learn about and advocate for federal legislation that affects veterans. Communicating with and educating lawmakers is vital to preserving and enhancing the VA health care system and other important institutions.
Otherwise, other voices will fill the silence.
For more information about DAV CAN, please visit davcan.org.
Editor’s Note: Data in the article updated on Jan 27, 2025